Meth Sores & Symptoms of Meth Use


Key Takeaways
- Meth sores are painful wounds caused by methamphetamine abuse - Jump to Section
- Meth sores look like rashes, cuts, blisters, or acne - Jump to Section
- Meth sores are caused by scratching, poor hygiene, and burns - Jump to Section
- Meth mites are hallucinations of bugs on the skin leading to scratching - Jump to Section
- Meth sores mainly form on the face and mouth - Jump to Section
- Signs include rapid speech, weight loss, and strange behavior - Jump to Section
What Are Meth Sores?
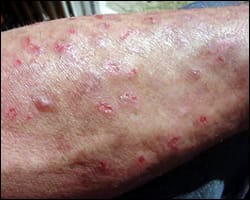
Meth sores are open wounds along that commonly develop on the arms, face, and/or throat. They develop when someone abuses methamphetamine or crystal meth.
It's a common skin condition among meth users caused by their drug's physical and psychological effects.
What Do Meth Sores Look Like?
Meth sores look different depending on their cause and whether or not they are infected. They are red and look like rashes, cuts, blisters, or chickenpox. Sores on the face or throat might look like acne.
In many cases, someone using meth will scratch and pick far more compared to when they're sober. This is because the drug increases their pain threshold.
When they realize there's a wound, the sores might develop a black or brown center and grow into a blister filled with pus.
If a person stops using meth and cares for his or her skin, sores will heal, scab over, and eventually fade. They can scar, depending on the severity of the sore.
What Causes Meth Sores?
The majority of meth sores are self-inflicted. Meth users itch or experience the sensation of bugs crawling on their skin (methamphetamine-induced self-excoriations).
Meth users overreact to the itching due to their paranoia and anxiety. Scratching in reaction to these two side effects aggravates the problem.
People who smoke crystal meth can also develop meth sores from glass tubes, which can become heated to the point of burning. This causes mouth and mucosa ulceration.
A combination of poor nutrition and less-than-adequate hygiene also contributes to skin fragility. This allows bacteria to enter the skin through the sores, causing infection.
What Are Meth Mites?
After several days without sleep, some meth users begin to hallucinate bugs crawling under their skin. These bugs are specifically called “meth mites,” "ice mites," or “crank bugs.”
Another term for meth mites is formication. It is a physical hallucination that makes people think they are covered in insects.
This physical hallucination can be triggered by meth use. People with "meth mites" often start itching and scratching excessively, leading to meth sores.
Where Do Meth Sores Form?
The Face & Skin
Meth users have an increased tolerance to pain. They can start picking and scratching at their skin without realizing they've hurt themselves. Meth sores can occur anywhere on the body, but they tend to be worse around the head and neck.
Not all meth users experience meth mites (formication). However, they're more likely to experience skin problems the more they use the drug.
Research shows about a quarter to half of all people dependent on meth experience hallucinations, psychosis, or mental deficits, including the sensation of bugs.8
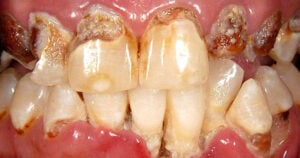
The Mouth (Meth Mouth)
Many people are familiar with the term “meth mouth” or know that people who use meth tend to have poor dental hygiene.
According to a 2015 study, 96 percent of meth users had cavities. More than half have untreated tooth decay. And about a third of meth users have six or more missing teeth.2
Meth mouth causes teeth to blacken, rot, and eventually fall apart. Doctors believe extensive tooth decay occurs due to:
- Long periods of poor dental hygiene
- Dry mouth
- Excess cravings for carbonated, sugary beverages
Signs of Meth Use
People who use meth often exhibit specific behaviors and symptoms, including:
- Constant, rapid speech
- Rapid weight loss and loss of appetite
- Sores or scars from scratching
- Paranoia and erratic behavior
- Extreme bursts of energy
- Dilated pupils and rapid eye movements
- Rapid breathing
- Mood swings and outbursts
- Unstable sleep schedule
- Tooth or gum decay
- Bad body odor
- Pale or blotchy skin
- Profuse sweating
- Grinding teeth
Tweaking and Crashing
Tweaking happens at the end of a meth high. It occurs when the drug cannot provide a "high" or euphoria. Once the high wears off, users are left with cravings and feelings of despair.
Signs of tweaking include:
- High-intensity cravings
- Powerful frustration and paranoia
- Hallucinations
- Imaginary bugs crawling on the skin
- Detachment from reality
- Insomnia
- Self-harm
Crashing is the first stage of meth withdrawal. It usually happens 1 to 3 days after the last use. It includes loss of energy and cognitive function.
Often, people sleep for one to three days during their crash. This can lead to high-intensity cravings, insomnia, depression, and hopelessness.
Methamphetamine Statistics
2.6
Million
People reported methamphetamine use in 2020.
23
Years Old
The average age of new methamphetamine users is 23.3 years old.
61
Percent
Of people released from treatment for methamphetamine relapse within the first year.
Treatment for Meth Sores & Meth Addiction
The best way to treat or cure meth sores is to stop using meth altogether. By quitting and making healthier life choices, the sores will heal over time.
Infected skin sores require medical attention. If a sore becomes infected, treatment will include antibiotics and/or draining the sore's abscessed part. The time it takes meth sores to heal depends on the severity of the sores and the person's immune system. Long-term use of meth tends to weaken immunity.
There are many meth addiction treatment programs. Some of these include:
Rehab
Meth rehab centers use different courses and frameworks for addiction recovery. They will usually conduct a consultation to understand the full scope of your needs before recommending a treatment plan. Rehab options can be inpatient or outpatient. Partial hospitalization programs (PHPs) and Dual diagnosis treatment are also available.
Cognitive-Behavioral Therapy (CBT)
In cognitive-behavioral therapy, healthcare specialists may suggest the Matrix Model. This is a 16-week approach for those who abuse methamphetamine. It is a comprehensive program, including behavioral therapy, family education, personal counseling, 12-step support, drug testing, and encouragement for non-drug-related activities.
Inpatient Treatment Centers
Detoxification and withdrawal are complicated and dangerous processes without proper medical supervision. Inpatient treatment centers provide that guidance by giving medical and psychological support during every step of recovery.
Currently, no drugs are available to counteract the effects of methamphetamines or those caused by long-term abstinence. However, the National Institute on Drug Abuse has conceived a method called MIEDAR (Motivation Incentives for Enhancing Drug Abuse Recovery). The incentive-based approach has been shown to encourage cocaine and methamphetamine abstinence.
Summary
Meth sores is a serious condition that may occur among meth users. They result in red and painful wounds around the body, usually in the face and mouth. With the right treatment plan, recovery is possible. If you or a loved one needs help with a substance use disorder, including meth use, contact an addiction specialist today.
- Grant, K., et al. “Methamphetamine-Associated Psychosis.” Journal of Neuroimmune Pharmacology, 2011.
- “Meth Mouth - American Dental Association.” Mouthhealthy.Org, 2015.
- “What Is the Scope of Methamphetamine Misuse in the United States?” National Institute on Drug Abuse, 2022.
- “Methamphetamine Trends & Statistics.” National Institute on Drug Abuse, 2020.
- Brecht, M., and Diane H., “Time to Relapse Following Treatment for Methamphetamine Use: A Long-Term Perspective on Patterns and Predictors.” Drug and Alcohol Dependence, Elsevier, 2014.
- "What are the long-term effects of methamphetamine misuse?" National Institute on Drug Abuse, 2022.
- Salamanca S., et al. "Impact of methamphetamine on infection and immunity." Front Neurosci, 2015.
- Rusyniak DE. "Neurologic manifestations of chronic methamphetamine abuse." Neurol Clin., 2011.